Data Sharing in Healthcare: The Benefits and Challenges
22 February 2024
The healthcare sector has witnessed a transformative shift towards shared data in recent years. There’s a growing recognition of the immense potential to improve patient care, streamline operations and manage rising population health concerns through shared records and integrated care systems.
However, along with the many advantages of sharing data, there are also potential risks that need to be addressed. Not just security and data privacy concerns, but also the lack of public engagement and education on the benefits of sharing healthcare data across authorised sectors.
This article delves into the key drivers, benefits and challenges of data sharing in the healthcare sector, and how it is revolutionising patient care across the industry.
Benefits of data sharing in healthcare
1. Improved Patient Care
Access to a patient's complete medical history allows healthcare providers to make more informed and personalised treatment decisions. With a few clicks of a button, they can quickly retrieve relevant health data, including allergies, medications, past test results, treatment plans, and more.
This reduces the need for patients to repeat their history, minimising the risk of unintentionally forgetting anything and ultimately improving the quality of care they receive.
2. Collaboration and Integration
Integrated health data also fosters collaboration among care providers, breaking down silos and promoting an integrated approach to care.
With seamless data access, the entire team can coordinate more effectively, leading to a holistic and patient-centred care experience.
3. Population Health Management
Data sharing supports crucial research and public health initiatives. Healthcare providers can leverage anonymised and aggregated data to track health factors, identify trends, and develop evidence-based strategies to tackle localised issues.
This wealth of information empowers healthcare professionals to proactively address emerging population health challenges.
4. Efficiency and Cost Reduction
Shared data can improve administrative efficiency by reducing paperwork, administrative errors, and the time required for to retrieve critical information. This, in turn, helps care providers reduce waiting lists and system pressures.
Having a comprehensive view of a patient’s health records also prevents medical errors. This reduces the likelihood of duplicate tests and procedures, minimising costs and enhancing overall efficiency.
The Challenges of Data Sharing
While these benefits showcase the positive aspects of data sharing in healthcare, it's important to also address the associated concerns and challenges.
Data privacy is a significant consideration in sharing healthcare data, which often contains sensitive and personal information, including medical history, diagnoses, treatments and genetic data.
Care providers must ensure that safeguarding measures, including advanced encryption, authentication protocols and strict access controls, are in place to ensure the confidentiality and integrity of patient data.
Using the appropriate legal basis when sharing data is also, of course, essential. When sharing for direct care the UK General Data Protection Regulation has a medical purposes clause that allows sharing without any other permissions needing to be sought. If the use is for purposes other than care, there are means that allow this for management of healthcare services, public interest and scientific research.
Clinicians must familiarise themselves with GDPR and the official regulations around data sharing, while patients should be made aware of how their data will be used, who will have access, and for what purposes.
By providing information about the benefits of seamless data access, such as improved care coordination and personalised treatment plans, providers can help patients understand the value of these systems. Educated patients are more likely to feel confident in the healthcare system's capabilities and take a more proactive approach to their own care.
How Graphnet Health protects patient data
At Graphnet, safeguarding patient data in our shared care record systems is paramount. We’ve established robust protective measures under our Information Governance (IG) framework, which controls the management and security of sensitive data. This includes clear access controls, thorough audits, encryption protocols and rigorous security testing.
We understand the importance of integrating data protection into our core operations. Following a ‘privacy by design’ approach, we align with all NHS guidelines on Information Governance, including the use of the Data Security and Protection Toolkit. Our management structure also includes a Senior Information Risk Owner and Caldicott Guardian, who are responsible for ensuring the confidentiality of health and care information.
Our integrated solutions are hosted on Microsoft Azure’s cloud platform, with servers located in the UK. We hold Cyber Essentials Plus certification and our security compliance team works continuously to meet Information Security and Data Quality ISO standards, regularly conducting scans and penetration tests to uphold system security.
Case Studies: Shared Data in Action
Improving maternal care at Cheshire and Merseyside
In a March 2023 report, the NHS outlined a three-year delivery plan to reduce health inequalities in maternal care, using shared population health data as a key tool. One region already putting this into practice is Cheshire and Merseyside.
The Cheshire and Merseyside Women’s Health and Maternity Partnership worked with CIPHA and Graphnet Health to develop an interactive pregnancy dashboard that would help tackle Covid-19 vaccination rates in pregnant people.
The dashboard pulled in a range of authorised health and care data from across the ICS, including:
- How many women were coming forward to be vaccinated
- Which stage of gestation they were in
- Age
- Ethnicity
- Any long-term conditions
- Socioeconomic residence
This information allowed the team to pull together a collaborative plan with community care services that helped engage the most deprived people in the region.
The project was – and continues to be – a success. By December 2022, the region’s vaccination rate for pregnant women had increased from 56.4% to 79.8%.
The dashboard is now being used to help tackle other women’s health issues, including increasing cervical screenings, reducing rates of smoking in pregnancy, and improving mental health care.
Sharing data to tackle fuel poverty health risks
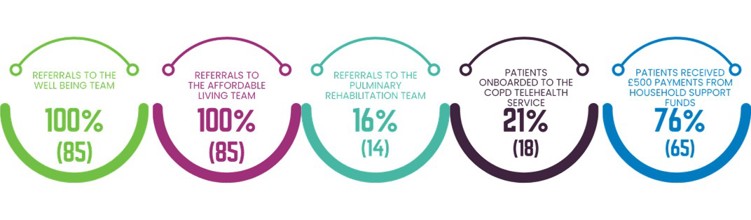
Cheshire and Merseyside ICB has since created a similar dashboard using Graphnet Health tools to help identify and target patients with respiratory conditions that may be exacerbated by living in a cold, damp home.
Shared data allowed the team to pinpoint a list of individuals who could benefit from a fuel poverty programme that combined health and social care. These patients were then contacted to obtain their explicit consent to share their data with other agencies who could help support them and their health through the winter months.
Get in touch to discuss how Graphnet’s shared data platforms can support you









